Research Topics
Opportunity Policy
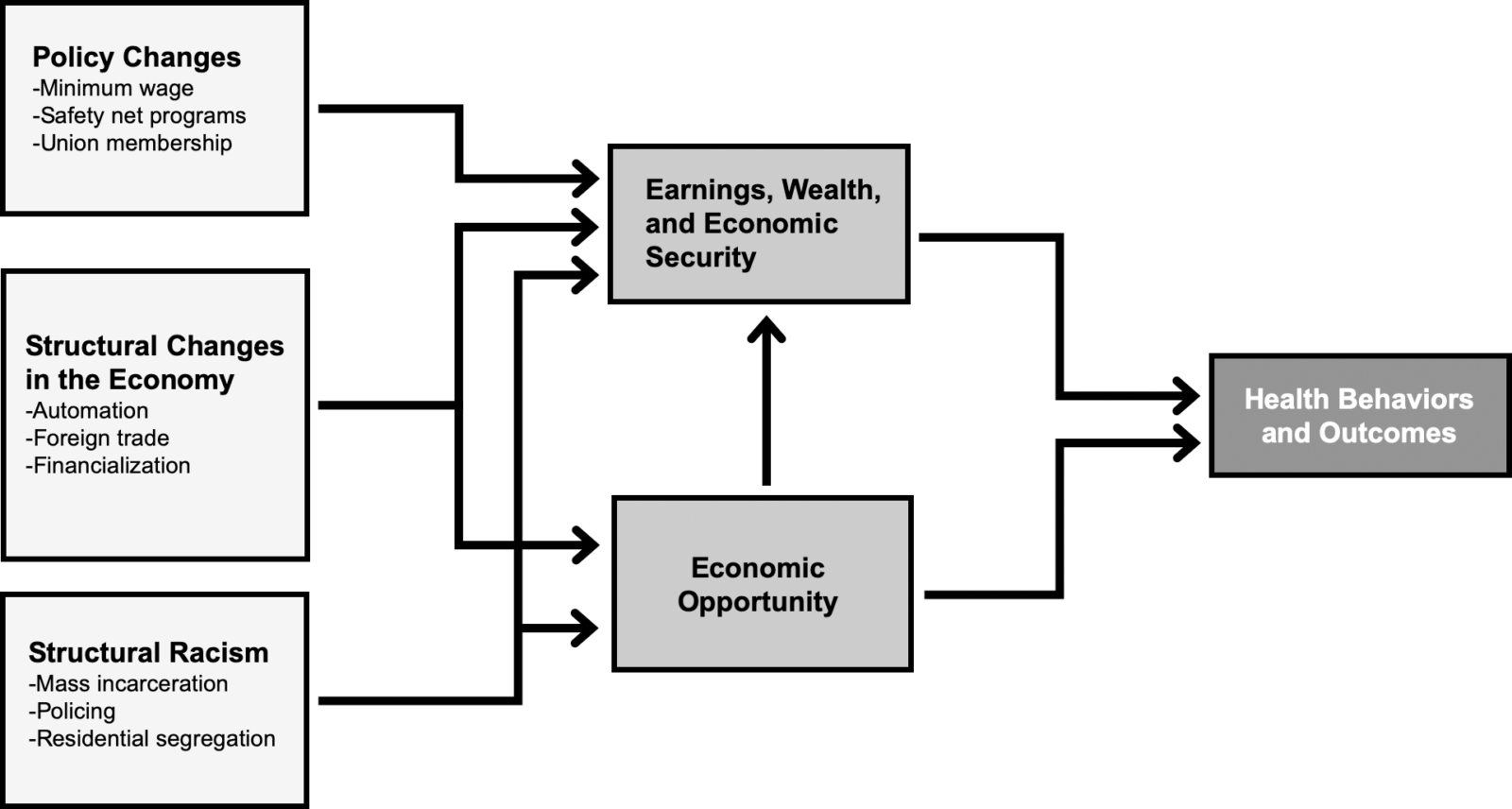
Research by our group and others has shown that higher economic opportunity is associated with better health outcomes. This brings up a critical question: what policies can help boost both economic opportunity and health? The science suggests several types of policies that can help meet these twin-goals. (The following list is not exhaustive. However, it provides a road-map of the range of interventions our lab is interested in.)
Investing in Young Children
Evidence shows that policies that increase early life access to high-quality preschool and healthcare lead to higher incomes and better health in adulthood. The same can be said for policies that reduce early life exposure to pollution. Policies that move children (and their families) to better neighborhoods have also been shown to lead to increased educational attainment and income later in life (e.g. the U.S. Housing and Urban Development’s Movement to Opportunity experiment). There is no doubt that extra support at a young age has positive lasting effects throughout one’s entire life course.
Invest in Education
Increasing access to high quality education has historically played a key role in boosting economic opportunity. Substantial research also shows that investing in education may improve health. Putting this together, policies that improve access to high quality educational opportunities (whether K-12, college, or vocational education) may help boost both opportunity and health for millions of Americans, particularly those with lower incomes.
Financial Support
Policies that provide additional financial support to those that need it can improve economic opportunity and thereby improve health. There is evidence that suggests minimum wage increases, increases in the Earned Income Tax Credit, and more generous unemployment insurance lead to fewer deaths from suicide among individuals with lower levels of education. These types of policies can help blunt the relationship between diminishing economic opportunity and poor health. There is also emerging evidence around the impacts of Universal Basic Income (UBI) and similarly designed cash transfer programs on health and educational attainment. Currently, there are a number of large randomized trials in progress being run across the country that will shed light on how effective these types of policies can be.
Job Re-Training
It is no secret that automation and technological advances have made certain types of jobs much harder to come by in America today. The case study of automotive assembly plant closures and drug deaths shows how critical these trends may be for public health. Similar adverse public health consequences have been demonstrated in areas where jobs have disappeared due to exposure to foreign trade. The U.S. Trade Adjustment Assistance (TAA), which aims to retrain workers who have lost their jobs due to foreign trade, has shown to have significant positive effects on employment and income from those who have benefited. Similarly, demonstration programs that provide occupational and soft-skills training for low-income workers have been shown to generate large, sustained impacts on earnings. Individuals served be this programs represent just a small fraction of workers whose jobs are threatened by automation and trade. Scaling them up could improve economic opportunity and health for a large number of Americans.
Improving Safety Net Program Design
Improving access to long-standing safety net programs such as Temporary Assistance for Needy Families, and the Supplemental Nutritional Assistance Program can help partially stave of economic insecurity – and the negative health consequences that arise from it – during hard times. “Administrative burdens” can make it hard for low-income individuals and families to sign-up, receive, and renew benefits. Interventions to reduce these burdens have been shown to increase program take-up rates, while policy designs that increase these burdens reduce take-up, even during times of great need.
Anti-Discrimination Policy
For marginalized population groups such as African Americans, improving health outcomes may additionally require supplementing universal economic and social policies with specific interventions to reduce long-standing, historically patterned barriers to economic opportunity. Longevity gaps between Black and white Americans continue to persist, and closely track with similar gaps in economic opportunity. Racial and ethnic disparities of the kind observed in our research require particular attention, including from policies that address discrimination in labor markets, criminal justice, and education.
Health Insurer and Health Care System Programs
There has been a recent push in the health care world to consider the social determinants of health. Some insurers and health care systems have created programs to address these social determinants, paving the way for improved economic opportunity and health for patients. Examples of these types of programs include improved access to housing and community health worker programs . The evidence base is still thin on what works and what doesn’t, but it does seem clear that we will have rethink how we pay for health care in order to make these programs work best for patients.
Developing New Approaches
Improving opportunity and health for all will requiring moving beyond what we know. We will need to develop and test next-generation programs and policies to move the needle. Our lab is at the forefront of these efforts. For example, we are collaborating with the Penn Urban Health Lab on a $10 million, NIH-funded study that will develop and test an unprecedented, multi-component intervention seeking to substantially improve health outcomes in Philadelphia’s poorest neighborhoods.
We are also committed to improving how we evaluate new policies. Our lab members have been among an influential group of scientists calling for the regular use of research methods (e.g., randomized control trials) when implementing new public policies. We have already been successful in this achieving this goal, convincing a large state to run a randomized trial of a controversial change to one of their social programs.
View Related Research